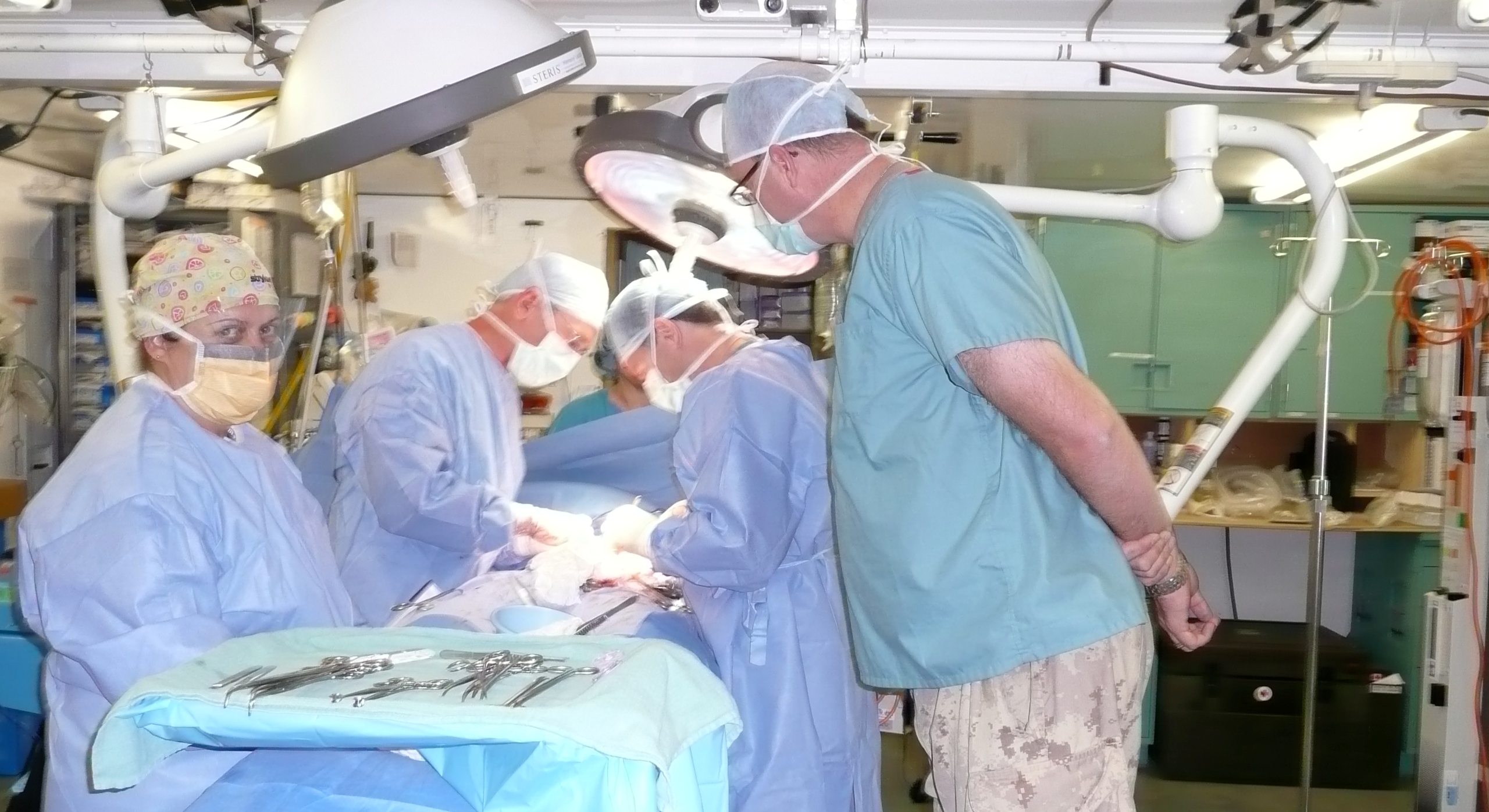
Remembrance Day is important to Stewart Hamilton, a faculty member and former trauma surgeon whose son currently serves with the Canadian military. In 2008, Hamilton did a multiple-week tour in Afghanistan as a civilian - an experience he says he will always remember.
Back in 2008, Canada had a lead role in staffing the hospital in Kandahar, Afghanistan. Because the Canadian military didn't have enough permanent medical and surgical staff to fully staff the facility, they asked for civilians to lend their services and expertise. Hamilton, a professor in the Department of Surgery, was happy to support the Canadian military and offered to go.
"I was there to support the Canadian mission and the people of Afghanistan in the middle of an insurgency. That was extremely rewarding - to know you could provide care to those who would otherwise never be able to get that level of care and medical assistance," said Hamilton.
Two trauma surgery teams were on site; one was made up of Canadian physicians, and the other included military physicians and surgeons from Denmark. Each team had a general surgeon, an orthopedic surgeon and an anesthesiologist. The first month Hamilton was there, the teams completed 133 surgeries - a record number at the time. The most common surgeries were for major chest, abdominal or orthopedic injuries - wounds resulting from the implosion of suicide vests or improvised explosive devices (IEDs), as well as gunfire, vehicular accidents and rocket-propelled grenades.
"The first surgery I did was an extremity injury - a high-velocity gunshot wound to the leg. We were successful in saving the leg. And the last big surgery I did was a high-velocity gunshot wound to the right lobe of the liver. In the end, the patient did well after multiple procedures.
"In between those cases, I did a number of trauma surgeries where Afghan civilians were hurt due to suicide vests exploding. The vests were meant to maim and do as much damage as possible. The vests would be loaded with ball bearings and sharp little wood screws. I remember one of my early cases, a 15 year-old boy who was hurt when a suicide vest blew. The shrapnel caused penetrating trauma to his chest and abdomen. He lost part of his colon and spleen, but in the end did well. His case was typical of the senselessness of it all."
Hamilton said 90 per cent of the surgeries were performed on Afghans, and about half of those were civilians - civilians who were going about their regular day-to-day activities, like going to get polio vaccinations.
"In the paper this week, I happened to see a piece where the Taliban blew up a polio clinic in the northwest state of Pakistan, and the exact same thing happened when I was in Kandahar. One Sunday, the Taliban sent a couple of suicide bombers into a polio clinic and murdered the two doctors who were vaccinating the local population. I recall that we had seven casualties out of that."
Hamilton also performed a number of surgeries on soldiers. But not everyone could be saved. In the five weeks Hamilton was in Kandahar, seven Canadians died from injuries stemming from IEDs.
The trauma surgery teams worked in a plywood hospital affectionately nicknamed "the Plywood Palace"' that had 16 beds, two operating theatres, a CT scanner, lab services and a blood bank. This included a "walking blood bank" - blood donations on demand from the soldiers on the base.
"All of the soldiers had their blood screened and typed, so that if there was a mass casualty situation, you could call in the troops to donate blood. In the five weeks I was there, we had the walking blood bank in operation four times."
Hamilton said he valued the opportunity to work with the outstanding people within the Royal Canadian Medical Service, who recently received the Dominique-Jean Larrey Award from NATO (the North Atlantic Treaty Organization) for their exceptional service. This award is NATO's highest honour for medical support and has only been awarded on one previous occasion. The hospital in Kandahar had a 97 per cent survival rate and was one of the busiest trauma hospitals in the world at the time.
"I valued their professionalism, their commitment to their mission and their commitment to always do their best job in difficult circumstances, at all hours of the day and night."
Hamilton is one of several faculty members who has worked or still works with the Canadian military. He notes the good working relationship and strong working agreement between the Faculty, Alberta Health Services and the Canadian Armed Forces with many military members "integrated into our regular staff." This gives military medical personnel the opportunity to gain experience in the civilian world.
"We have a fairly active, very big trauma service within the city of Edmonton," said Hamilton. "We tend to see vehicular traumas involving cars and ATVs, and also have our share of gunshot wounds and stabbings, so military medical personnel are able to gain experience that counts for when they are in a war zone.
"The experience in Kandahar was an opportunity to give back and to support the Canadian military. I continue to be impressed with the Canadian military in general and the Royal Canadian Medical Service in particular. It was a real privilege to work with them - they are simply an amazing team of people."